Answer:
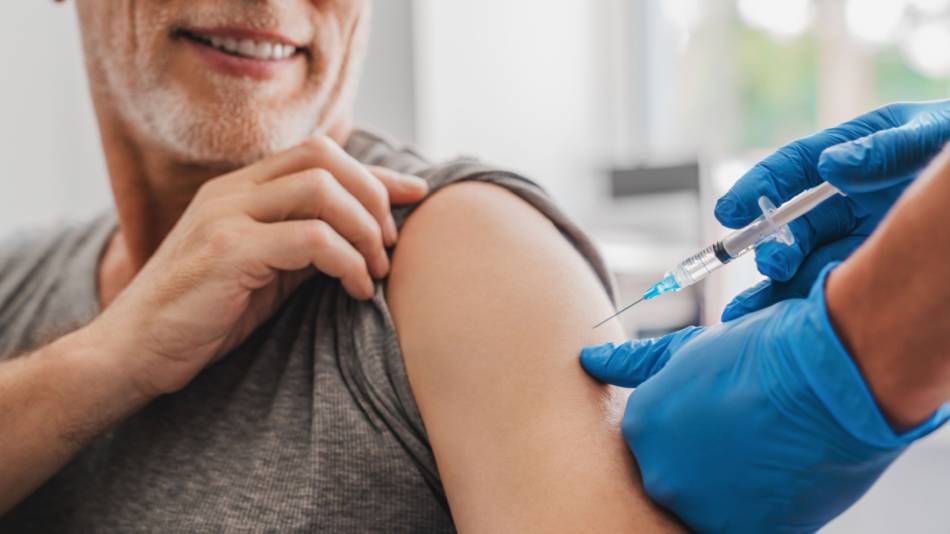
On September 11, 2023, the FDA approved and authorized for emergency use three updated COVID-19 vaccines to target commonly circulating variants based on recommendations made by its vaccine advisory committee (FDA News Release, 9/11/2023).
Sign in as a member to learn how the updated vaccines differ from each other (including efficacy and side effects), who can get them, who should not get them, who should not get additional doses, and where to get them.
Join today to unlock all member benefits including full access to all CL Answers and over 1,400 reviews.
Join NowAlready a member? Sign In Here.
Join now at www.consumerlab.com/join/







Submit your comment
This feature is restricted to active members.
Join now to add comments and get all member benefits, including over 1,400 reviews.
Join NowAlready a member? Sign in here.