Our Members Asked:
Which is the best mask to prevent COVID-19 and how do cloth, disposable, N95, and KN95 masks compare? How can I stop glasses from fogging?
Answer:
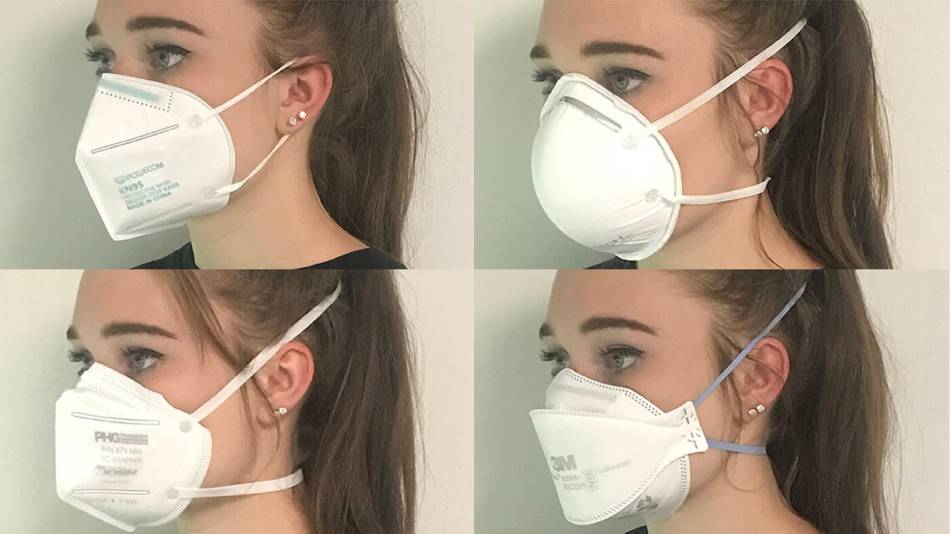
N95 masks are the gold standard, but well-fitting, high quality KN95 masks are also a good option. Disposable surgical masks are also readily available but tend to leave gaps between the mask and face, reducing their usefulness (although there are ways to improve it).
Sign in as a member to see ConsumerLab's Top Picks among N95 and KN95 masks.
Masks can be used alone or, for increased protection, particularly for the eyes, with a face shield — which we have also reviewed.
Here's what we cover in this answer:
- Why and When You Should Wear a Mask
- How N95and KN95 Masks Compare
- Best N95 Respirators
- Best KN95 (Respirator) Masks
- Best Disposable Surgical/Medical Masks
- Cleaning and Caring for Masks
- How to Improve Mask Fit to Reduce Leakage
- Does Double Masking Help?
- How to Reduce Eyeglass Fogging
- Concerns About Co2 Build Up
- Concern with Inhaling Microplastics and OPEs
- Are Copper Masks Better?
- What Masks Protect Against Wildfire Smoke?
Why and when you should wear a mask
While vaccination to protect against COVID-19 has led to a decreased need for masking, the CDC still recommends wearing a mask as an additional prevention strategy to reduce the spread of the virus to others when worn by someone with an infection, and to protect wearers from breathing in infectious particles from people around them. It advises that use of masks may be considered when 1) respiratory viruses are causing a lot of illness in your community, 2) you or the people around you were recently exposed to a respiratory virus, are sick, or are recovering, or 3) you or the people around you have risk factors for severe illness, such as women who are pregnant, young children, older adults, and people with a compromised immune system.
As wearing a mask may reduce the amount of virus to which a wearer is exposed, it has been postulated that even if a mask-wearing person becomes infected, the reduced viral load to which they were exposed may mean that they suffer a milder disease. For example, on cruise ships with COVID-19 outbreaks, the majority of infected patients (81%) were asymptomatic on a ship that had provided surgical masks to all passengers and N95 respirators to staff compared to only 18% of cases being asymptomatic on a cruise ship without masking (Gandhi, J Gen Intern Med 2020; Gandhi, N Engl J Med 2020).
Another benefit of wearing a mask is that, due to the heat and moisture of exhaled breath, masks have been shown to increase the humidity and temperature of inhaled air, which, researchers have proposed, may reduce the risk of respiratory infections such as COVID by promoting the clearance of pathogens in the lungs (Courtney, Biophysical J 2021).
Any benefit to wearing masks at home?
Although CDC guidelines do not currently include the use of face masks at home, the rate of transmission from one household family member to another was 79% lower when members wore face masks prior to the first member developing COVID-19 symptoms, according to a study of 124 families in Beijing in which there was at least one infected person. Overall, there was a 23% rate of transmission of COVID-19 from an infected family member to another, but this was no lower when mask wearing began after the first member developed symptoms. These results are consistent with the fact that viral load is highest two days before symptoms and on the first day of symptoms. Daily use of disinfectants reduced transmission by 77%. Transmission rates were four times higher if the primary case had diarrhea and 18 times higher when there was frequent daily close contact (less than 3 feet apart). The researchers recommended use of face masks in families in which a member has been at risk of getting infected. In China, over 70% of transmission occurred within families (Wang, BMJ Global Health 2020).
Which masks protect you best?
The CDC advises that the most protective masks are NIOSH Approved filtering facepiece respirators (like N95 respirators), followed by international filtering facepiece respirators (like KN95 respirators), surgical/disposable masks (although they provide far less protection than N95 and KN95s), and lastly, cloth masks (CDC 2024).
A study that evaluated how well masks protect the wearer from breathing in small particles (ranging in size from 0.02 to 0.6 microns) and factored in the fit of the mask as well as its filtration efficiency found that a NIOSH approved N95 (3M 9210) had the highest filtration efficiency at 98%, followed by 80% for a medical procedure mask with ear loops (Cardinal Health) with nylon hosiery placed over it, and 71.5% for a surgical mask with ties. [Note: The filtration efficiency of the medical procedure masks can range dramatically depending on how it was worn.] The filtration efficiency was 74% for a 2-layer woven nylon mask with ear loops (Easy Masks LLC) with an aluminum nose bridge and nonwoven filter insert which, interestingly, had a slightly higher filtration efficiency after being washed once, 49.9% for a folded, cotton bandana, 39.3% for a single-layer woven polyester/nylon mask with ties (Renfro Corporation), 37.8% for a single-layer woven gaiter/neck cover balaclava bandana MPUSA LLC), 28.6% for a nonwoven polypropylene mask with fixed ear loops (Red Devil Inc), and just 26.5% for a 3-layer woven cotton mask (100% cotton) with ear loops (Hanesbrands Inc) (Clapp, JAMA Intern Med 2020).
How N95 and KN95 Masks Compare
NIOSH approved particulate N95 respirators have been tested by the National Institute for Occupational Safety and Health, a division of the U.S. CDC. They must meet certain minimum criteria, including a particular filtration efficiency of at least 95%, an inhalation resistance of < 25 mm H20 and an exhalation resistance of <35 mm H20 (these are measures of how difficult is to breath in and out while wearing the respirator). Unlike cloth masks, NIOSH approved N95s are also required to attach to the head with head straps, rather than ear loops, as head straps can provide a more secure fit and reduce gapping.
KN95 respirators, the Chinese "equivalent" of N95 respirators, must meet similar standards, including a particular filtration efficiency of at least 95%, and limits for inhalation and exhalation resistance. They are not required to have head straps (most have ear loops), although some do. Be aware that, during the pandemic, there have been many reports of counterfeit KN95s sold in the U.S., so you need to be careful where you buy KN95s. As of December 2021, sales in the U.S. of counterfeit N95 and KN95 respirations continue to be a problem, according to the CDC. The agency provides tips for spotting counterfeits and updates its page with examples of counterfeit respirators. As discussed below, although ConsumerLab's Top Pick among KN95 respirators can be found on Amazon, we do not recommend purchasing it there (as the CDC has indicated that there could be counterfeits), but it can be purchased through an authorized dealer.
(For more about the differences between N95s and KN95s and quality concerns, see Are KN95 respirators as good as N95s?).
General Precautions
Be aware that, as noted by the FDA, people with chronic respiratory, cardiac, or other medical conditions that make breathing difficult should consult with their healthcare provider before using an N95. Also be aware that having facial hair can compromise the fit and protection provided by N95s (see below for more about this), and that N95s are not designed to be worn by children. N95s with exhalation valves should not be relied upon when sterile conditions are needed, and are not recommended for protecting from COVID-19.
Fit and Use
In healthcare settings such as hospitals, people using N95s have to undergo regular fit testing using sodium chloride particles to ensure the N95 they use is the proper size and provides a tight seal to prevent air leakage. This test cannot be performed at home, but to ensure the best fit possible, make sure the N95 you choose fits snugly, without gaps, around your nose, mouth, cheeks and chin. Some manufacturers also suggest holding your hands in front of the mask and above the nose bridge (without touching the mask) once it is in place exhaling to check and see if you feel air leakage. You may find instructions for doing this user seal check on the packaging of some N95s.
Facial Hair and N95s
As noted above, facial hair can interfere with the fit, and therefore the protection provided by, N95s. Being clean-shaven while wearing an N95 is best, but facial hair may be acceptable if it does not come between the skin and the edge of the respirator where a snug seal should form. The CDC provides an infographic of facial hair styles for clarification.
A study that investigated the effects of beards on the filtration efficiency of an N95 (3M Model #8210) found that average filtration efficiency decreased from 98.9% when clean-shaven to about 95% with beards of various lengths (a little less than ½ an inch up to 1 ½ inches in length). Despite this, it found that the N95 still offered better protection than KN95s or surgical masks for beard lengths up to ½ inch. KN95 filtration efficiency also decreased from about 95% clean-shaven to about 40 - 70% for the longest beard length of 1.2 inches but provided better protection than a surgical mask with ear loops (Medline Industries) or a 3-ply 100% cotton mask with ear loops and adjustable nose piece (Hanes). Covering beard hair with a large yoga-style exercise resistance band underneath respirators improved filtration efficiencies, however these bands appear to be quite large and may be uncomfortable or not practical to wear (Chen, Expo Sci Environ Epidemiol 2021).
How to reduce air leakage around a mask
Air leakage around a mask reduces the level of protection it provides you and those around you. There are several ways to reduce air leakage, as discussed below. Also be aware that if you are infectious, the area of your face beyond a leak, including eyeglasses, may become contaminated due to exhaled droplets, as demonstrated in OSHA study (Stephenson, medRxiv 2021 -- preprint).
Knotting ear loops
The fit and filtration efficiency of medical procedure masks with ear loops can be significantly improved by knotting the ear loops and then tucking in and flattening the extra material close to the face (see illustration), according to research conducted on manikins by the CDC. This was shown to reduce exposure to aerosols from a cough by 64.5%.
Double masking
Wearing a medical mask (i.e., a blue "procedure" mask) under a cloth mask improves protection, (likely by minimizing leaks between the medical mask and skin), but wearing a medical mask over a cloth mask has less benefit. A study found that wearing a medical mask under a cloth mask increased the filtration efficiency of cloth masks (which, alone, were 41 to 44% efficient), as well as medical masks (which, alone, were 43 to 62% efficient). Adding a medical mask beneath a cloth mask increased fitted filtration efficiencies to 66% for a simple cotton ear-loop mask, 77% for a cotton bandana, and 81% for a gaiter. Doubling a medical mask was not as effective, nor was doubling cloth masks — which also reduced breathability (Sickbert-Bennett, JAMA Intern Med 2021).
Try not to bend over while wearing a mask
Researchers at Columbia University who were fit testing N95 respirators found that normal breathing and talking did not negatively affect mask fit, and turning the head from side to side slightly improved fit (perhaps due to tightening). However, moving the head up and down slightly worsened fit, and bending over decreased proper fit by as much as 50%. The researchers suggested kneeling rather than bending over when wearing a mask (Chen, medRxiv 2020 -- preprint).
Mask fitters
Masks fitters are a "frame" that can be placed over masks to improve the fit and "seal" of the mask against the face to reduce air leakage and increase inhalation filtration efficiency. Using mannequins that could "breathe" (as shown in the image below), researchers at the University of Wisconsin-Madison found that placing either of two marketed mask fitters over a variety of masks increased inhalation filtration efficiencies from 52% to 63% for a 3-ply spunbond polypropylene mask, from 44% to 91% for a surgical mask, and from only 18% up to as much as 95% for a 3-ply disposable non-medical mask with a melt-blown polypropylene center. Fix the Mask ($30 for a 2-pack) tended to be slightly more effective than Badger Seal ($9.99 for 1), but the difference was not statistically significant (Rothamer, medRxiv 2021).
How to reduce eyeglass fogging from masks
Lens fogging may be minimized by rinsing lenses with highly diluted liquid soap and then air drying (stand lenses up so excess drips off) (Hu, J Emerg Nurs 2020). This leaves a surfactant film that reduces surface tension and causes water molecules to spread out evenly into a transparent layer, reducing fogging (Margrain, Ann R Coll Surg Engl 2011). Anti-fogging sprays and wipes are also sold, but be sure to follow directions and allow liquids to dry before wearing to avoid eye irritation or injury from the liquid. (A CL member reported severe eye irritation after using JAWS Spit Gel which seems to have gotten into his eye after a COVID nasal test that caused eye tearing) (Peng, Cornea 2006). Eye injury has also been reported in healthcare workers in China who used anti-fog spray on medical goggles (Hu, J Emerg Nurs 2020).
Double-sided tape strips, such as MaskTite Adhesive Strips, can also be used to seal the edges of masks around the eyes and nose to reduce fogging. ConsumerLab purchased these strips ($14.20 for 36 strips on Amazon) and tried them with a disposable mask while wearing glasses, and they did reduce fogging when properly affixed along the tops and sides of the mask.
Re-using N95s?
In general, N95s should not be reused, as the CDC notes that "Previously worn N95 FFRs can serve as a source of pathogens, which can be transferred to the wearer." However, in times of crisis or when supplies are not available, the CDC advises a single N95 respirator may be reused up to, but no more than, five times. It also advises healthcare workers "wear one N95 FFR each day and store it in a breathable paper bag at the end of each shift with a minimum of five days between each N95 FFR use, rotating the use each day between N95 FFRs," noting that this "will provide some time for pathogens on it to "die off" during storage."
Sign in as a member for details about a study that evaluated the loss of filtration efficiency after multiple uses of N95 masks.
Preventing mask-related skin irritation and acne
Keeping masks clean can also help prevent skin irritation, acne, and other skin conditions that can be caused by or exacerbated by wearing a mask, including eczema (contact dermatitis), rosacea, and folliculitis (inflammation/infection of hair follicles). Although the term "maskne" has become a common term to describe skin irritation and eruptions after wearing masks, contact dermatitis appears to be the most common skin irritation associated with wearing masks. All of these conditions can be aggravated by humidity within the mask, increased bacterial load on the skin, and friction from mask material. In addition to replacing masks regularly, dermatologists recommend applying light moisturizer 30 minutes before putting on your mask and maintaining good oral hygiene to help minimize the risk of skin irritation. You can find more information and the full list of tips for skin care when wearing masks in this article (see "General measures to prevent PPE related facial dermatoses") (Rud, BMJ 2021).
Effect on breathing function and potential carbon dioxide buildup
When wearing an N95 respirator or a well-fitted mask with high blocking efficiency there can be some carbon dioxide buildup inside the mask over time (Sinkule, Ann Occup Hyg 2013). According to researchers at Stanford University, N95 masks are "are estimated to reduce oxygen intake by anywhere from 5 to 20 percent. That's significant, even for a healthy person. It can cause dizziness and lightheadedness." However, a small study in the U.S. found that wearing an N-95 mask for up to one hour did not cause any significant adverse effects in healthy healthcare workers performing moderate activities, despite significantly decreased inhaled oxygen and increased inhaled carbon dioxide levels (Roberge, Respir Care 2010). A representative from the CDC told Reuters.com that "...the level of CO2 likely to build up in the mask is mostly tolerable to people exposed to it. You might get a headache but you most likely [would] not suffer the symptoms observed at much higher levels of CO2. The mask can become uncomfortable for a variety of reasons including a sensitivity to CO2 and the person will be motivated to remove the mask. It is unlikely that wearing a mask will cause hypercapnia [elevated blood levels of carbon dioxide].
On the other hand, surgical masks (also known as medical masks), which are inherently not as well-fitting as N95 respirators, do not lead to CO2 intoxication or oxygen deficiency, as noted by the World Health Organization. Several studies have demonstrated this. For example, a study among 20 healthy adults showed that moderate exercise (walking on a treadmill) for one hour while wearing a surgical mask led to only slight, clinically non-significant changes in CO2 levels (as measured on the skin) compared to exercise without a mask (Respir Physiol Neurobiol 2012). Even during vigorous exercise (cycling to exhaustion, an average of about 10 minutes) a study among 14 healthy men and women showed that wearing a disposable surgical mask or a three-layer cloth mask (Washable 3D Face Mask, TriMax Sports Inc. — made with bamboo charcoal cloth, non-woven fabric, and Lycra) had no effect on blood or muscle oxygenation or exercise performance compared exercising without a mask (Shaw, Int J Environ Res Public Health 2020).
Furthermore, a study of 10 healthcare workers (including individuals with controlled asthma and four smokers), found that wearing a surgical mask (AFLUID, made of three layers of polypropylene and one layer of liquid resistant polyethylene) continuously for four hours did not reduce breathing function (Ciocan, Med Lav 2020). Additionally, older adults who wore a three-layer disposable nonmedical face mask with ear loops (Boomcare DY95 model, Deyce Leather Co Ltd) for one hour showed no decline in self-reported blood oxygen levels (as measured by pulse oximeter) (Chan, JAMA 2020).
Another study showed that, even among older adults (average age 71) with breathing difficulty due to severe chronic obstructive pulmonary disease (COPD), wearing a surgical mask during a six-minute walk test did not result in any major changes in CO2 retention (Samannan, Ann Am Thorac Soc 2020). The researchers suggested that discomfort while wearing a surgical mask might be caused by the increased warmth of facial skin and inhaled air inside the mask, which may trigger sensations of anxiety or claustrophobia in some people.
The CDC advises that face masks should not be placed on children under the age of two, anyone who has trouble breathing, or anyone who would not be able to remove the mask without assistance.
Inhalation of microplastics and OPEs
Concern has been raised about the risk of inhaling microplastic particles when wearing a mask made of polypropylene or other materials containing plastics. A study in China found that most masks increased the inhalation of fiber-like microplastics but notably decreased the risk of inhalation of spherical particles. While some evidence has suggested that fiber-like microplastics may be more toxic to animals than spherical microplastics (Ziajahromi, Environ Sci Technol 2017), the investigators concluded that, overall, inhalation of microplastics from masks is a small problem compared to the risk of spreading COVID-19 without a mask, as people already regularly inhale high amounts of microplastics from the air, with or without a face mask.
The study found that only N95 respirators reduced the risk of inhaling fiber-like microplastic particles compared to not wearing a mask, while a nonwoven mask, a fashion mask, and a cotton mask increased it by 17%, 41%, and 54%, respectively, surgical masks increased it by about 4% to 73%, and activated charcoal mask increased it by 117%. Inhalation of spherical microplastic particles was reduced by about 47% to 96% for all masks compared to not wearing a mask.
Disinfecting any of the masks with UV irradiation, alcohol, air blower treatment, washing with soap and water, or exposure to sunlight increased the microplastic inhalation risk compared to untreated masks, although the risk was only small following washing with water and was lowest following exposure to sunlight. Alcohol disinfection increased the risk of microplastic inhalation most significantly (Li J Hazard Mater 2020).
Polypropylene and other plastic materials used to make KN95 respirators, medical, surgical and other types of masks are often treated with organophosphate esters (OPEs), which act as fire retardants and improve flexibility. These chemicals are used in a variety of household materials such as clothing and carpeting and are found in drinking water and foods (which are now the largest source of exposure (Gbadamosi, Sci Total Environ 2021). High concentrations and prolonged exposure to OPEs through ingestion, inhalation or skin contact have been linked with cancer and may have other adverse effects, such as endocrine disruption, kidney and liver toxicity, and toxic effects on the nervous system.
An analysis conducted in Spain of 21 masks showed that all contained OPEs (KN95s contained the most), but when worn for a single use (four hours) in a moderate temperature (62°F), KN95s, FFP2s (the European equivalent of an N95) and surgical masks would increase an average-sized adult's daily exposure to OPEs (through inhalation) by about 10% -- and when added to average estimated total daily exposure of OPEs, levels of risk were still below those of acceptable risk. No inhalation of OPE compounds was observed with the fabric masks. The researchers advised that filtering facepiece respirators (such as KN95s and FFP2s) should still be used "in situations of relatively high risk of viral inhalation, such as poorly ventilated indoor public spaces." (Fernandez-Arribas, Environ Int 2021).
Disposable "non-surgical" masks vs. surgical masks
Disposable face masks are now widely in stores and online and typically consist of one to three layers of non-woven, blue or white material such as polypropylene and usually have elastic ear loops (which, as noted above, do not provide the snug fit that masks with ties or head straps can). Although some disposable masks sold to consumers may appear similar to surgical masks they are not FDA regulated and are not required to meet the same standards. More importantly, neither surgical masks nor non-surgical disposable masks are designed to protect the wearer, but to reduce the number of droplets and aerosols from the wearer. Both the FDA and CDC emphasize that, due to leakage that can occur around the edges of surgical masks, they "...do not provide full protection from breathing in airborne pathogens, such as viruses." The main function of surgical masks is to provide a barrier from fluids, splatter and droplets that may contain viruses and bacteria. For this reason, a well-constructed, properly fitted multilayer cloth mask may be a better option.
The material used for surgical masks must meet certain standards (known as ASTM F2100-19) for bacterial and particulate filtration efficiency, differential pressure (breathability), resistance to penetration by synthetic blood, and flammability as outlined by the American National Standards Institute (ANSI). During the COVID-19 epidemic, the FDA has given emergency use authorization (EUA) for additional surgical masks that have not been FDA-cleared, although these masks must also meet certain ASTM standards. Surgical masks from China are not eligible for FDA authorization (the reason for this is not explained).
While non-surgical disposable masks sold to consumers are not FDA regulated and are not required to meet the same ASTM standards as surgical masks, some of those sold online or in pharmacies or grocery stores claim to meet ASTM standards. However, these masks cannot make any claims to meet a NIOSH filtration efficiency standard, as such claims only apply to respirators (see further below).
Be aware that while disposable and surgical masks may list ASTM filtration efficiencies, these mask cannot make any claims to meet a NIOSH filtration efficiency standard, as these claims only apply to respirators (see below).
See How to reduce air leakage around a mask above for tips on improving the filtration efficiency of surgical and medical masks.
Are KN95 respirators as good as N95s?
N95 and KN95 masks (or, more technically, respirators) are designed to protect you, as well as others around you. Both are supposed to filter 95% of particles down to 0.3 microns. However, as discussed below, this isn't always the case with widely sold KN95 masks (which are designed to meet Chinese, rather than U.S. specifications). In addition, while N95 respirators attach with head bands to help ensure the best fit, most KN95s attach with ear loops, which may cause a loose or improper fit, and allow for air leakage. A study of N95 and KN95 respirators have shown that mask performance depends, in part, on the tightness of the contact between the material and the facial skin and masks that tied around the head outperform those with elastic ear loops (Sickbert-Bennett, JAMA Intern Med 2020). As discussed above, how you move while wearing a mask may also affect fit.
Tests of KN95s from China by the CDC show that the filtration efficacy of some KN95 masks is 95% or higher but can be as low as 5.3%. Furthermore, tests by ECRI, an independent, U.S. based non-profit organization that evaluates equipment for hospitals and healthcare systems, showed that 5 of 11 KN95s did not meet the filtration efficiency standard of 95%. ECRI also found large variations in filtration efficiencies of KN95s within the same lot from a single manufacturer, suggesting quality control issues. (You can download ECRI's test results, which includes manufacturer information and photos of the respirators tested by clicking on "PPE Testing Report" on this page on ECRI's site).
Nevertheless, due to the previous shortage of N95 masks, in April 2020 the Occupational Safety and Health Administration (OSHA) provided guidance that KN95 masks certified to China's GB2636 standards of 2006 or 2019 (imprinted on masks as "GB2626-2006" or "GB2626-2019") "will provide greater protection than surgical masks (i.e., facemasks, other than surgical N95s[3]), homemade masks, or improvised mouth and nose covers, such as bandanas and scarves." Caution: You should not buy a KN95 mask that does not have its GB2626-2006 or GB2626-2019 imprinted on it.
Buying a KN95
Starting in 2020, the FDA published and maintained a list of N-95 and KN95 respirators from China given emergency use authorization (EUA) from the FDA during the pandemic. However, as of July 6, 2021, due to the increased supply and availability of NIOSH-approved respirators, the FDA has revoked its authorization of non-NIOSH approved respirators manufactured in China for healthcare workers. Respirators with previous EUA status may still be marketed to the general public, but must be labeled as face masks, rather than respirators.
Update: On August 25, 2021, the FDA announced that NIOSH approval of N95 respirators made by Chinese manufacturer Shanghai Dasheng has been revoked due to serious concerns about the quality of these products, noting "the company did not implement, maintain, and control a quality management system." It advised healthcare workers stop using N95 respirators made by Shanghai Dasheng and intended for emergency use, including several sold under other brand names (see the FDA notice for details).
Avoid Counterfeit Respirators
Signs of a counterfeit respirator include no approval number or NIOSH markings, decorative fabrics or add-ons, and claims of being approved for children. The CDC publishes a list and images of dozens of counterfeit and falsely marketed respirators. In December 2021, the CDC added the SafeShield FS-N95 and Megha International's N95 to its list, both of which claim to be NIOSH approved but are not (CDC December 2021).
Other respirators
Before N95 respirators became more available, the United States Department of Labor, noted that healthcare workers who were unable to obtain N95 respirators could use R95, R99, P95, P99, P100 and others respirators. Like N95 masks, these are expected to filter out a minimum of 95% of particles of the most penetrating size, and those ending in a "99" or "100" filter out at least 99% or 99.97%, respectively, of such particles but can be more difficult to breathe through. R95 and P95 masks are typically used for protection when working with oil-based substances like fuel, paints, solvents, or pesticides. N95s are not resistant to oil, R95s are "somewhat resistant" and P95s are "strongly resistant to oil or oil proof," as shown in the CDC's infographic about these types of masks. If considering an alternative respirator, make sure it is NIOSH approved. Respirators with exhalation valves should not be used when trying to protect others. (See a video demonstration by researchers at Florida Atlantic University of how aerosols can spread when coughing while wearing an N95 mask with a valve).
KF94 respirators from Korea are often promoted as the Korean "equivalent" to N95 respirators, but this is not quite accurate. Although they can have relatively high filtration efficacy, KF94 masks are considered "public use" respirators and are not held to the same performance standards as Korea's Special 1st class "occupational use" respirators (which are considered to be roughly equivalent to NIOSH approved N95 masks). KF94 respirators are designed to have a filtration efficacy of 94%, and CDC tests of one brand of KF94 found its filtration efficacy to be even higher (99.85 to 99.94%). However, unlike all NIOSH-approved N95s (which attach with head bands), KF94 respirators attach with ear loops, which, the CDC points out, may compromise their fit and efficacy. The CDC did not perform fit testing on the KF94s it tested and noted a lack of information about manufacturing quality control. In addition, unlike surgical N95 respirators, KF94 respirators are not considered fluid resistant (Kim, J Korean Med Sci 2020).
Electrical air purifying respirators that mimic powered air-purifying respirators (PAPRs) are available on Amazon, ranging in price from about $60 to $100, but these devices would not be suitable for preventing the spread of COVID-19 among the general public. These devices include a portable high efficiency (HE) filter that can be connected to a face mask via a flexible hose/air duct to supply fresh air to the wearer. By ventilating air from the HE filter to the mask, these devices should create positive air pressure. This means that air exhaled by the wearer would leak out of the mask. Consequently, these devices might protect the wearer if the ventilation is strong enough, but they would not protect individuals nearby the wearer.
Furthermore, unlike NIOSH-certified PAPRs, which are rated as being more effective than N-95 masks, available electrical air purifying respirators do not appear to be certified. Therefore, it is uncertain if these devices even help protect the wearer. In addition, similar to other personal ("wearable") air purifiers, these devices might not be permitted on airplanes, as security officers can confiscate these devices if they feel they are unsafe or cause a threat.
Are copper masks better?
Copper has been shown to inactivate a wide variety of bacteria and some viruses, typically within minutes to hours of contact, and a study found that SARS-CoV-2 (at about 72°F and 40% relative humidity) was undetectable on copper after four hours (van Dormalen, NEJM (correspondence) 2020). There do not appear to be studies showing how effective masks made with copper or copper infused fabric are against SARS-Cov-2. However, preliminary research with other viruses suggests a possible benefit. A study funded by the maker of copper masks (Cupron) for healthcare and institutional use, showed that an N95 mask with two added layers of copper oxide infused material (polypropylene fabric containing 2.2% weight/weight copper particles) had a similar filtering efficacy as a regular N95 mask, but was much more effective in inactivating human influenza A virus (H1N1) and avian influenza virus (H9N2) (Barkow, PLoS One 2010).
Some concerns have been raised about the safety of copper masks and the possibility of breathing in copper particles. While we don't have safety information for specific products, laboratory studies that measured the amount of copper released from copper oxide impregnated masks during 5 hours under simulated breathing conditions was far below the respiratory copper permissible exposure limit (PEL) set by the USA Occupational Safety and Health Administration ("OSHA") (Borkow, Curr Chem Biol 2012).
How to protect yourself from COVID-19 in a car
Preliminary research suggests that viral loads can quickly build up within a closed car, even during rides as brief as 15 minutes. Wearing a mask, as well as a face shield, are good first steps to help protect yourself and others. When there are two people in a car (one driver and one passenger) seating the passenger in the back seat on the opposite side of the driver creates the most distance between them. To increase ventilation, computer modeling research shows that riding with all windows down is most effective. Since this isn't always practical, the next most effective way to increase ventilation is by opening one window in the back and one in the front, opposite of where the occupants sit, creating airflow across the interior of the car. Keeping all the windows closed and running the air-conditioning, is least effective (Mathai, Sci Adv 2020). Keep in mind that none of these steps eliminate the risk of infection.
How to improve safety for bus passengers and drivers
A study of aerosol flow on a school bus and transit bus that were driven under real-world conditions showed that mask wearing and ventilation can significantly reduce exposure to aerosols for passengers (Edwards, Aerosol Sci Tech 2021). Based on their experiments, the researchers recommended the following tips to help reduce exposure to aerosols for bus passengers:
- Require all passengers and drivers to wear masks on buses. Even a cloth mask that's 50% efficient can reduce particles released from a cough by 50% and reduce their dispersal by several feet.
- Open windows partially or fully. This can reduce airborne particles by 50% to 80%.
- Consider seating arrangements that only allow for same household or same cohort passengers to sit together.
- Social distancing of six feet is not practical on most buses, but any extra distance allows the air movement to reduce exposure to infectious particles.
For bus drivers, the researchers recommended risk could be reduced by using a dashboard fan to create airflow in the driver seat area. They also noted that, when safe to do so, opening all transit bus doors at every stop would allow for better air exchange.
What masks protect against wildfire smoke?
Cloth masks, including those with sewn-in or removable filters, should not be relied on for protection from wildfire smoke, according to the CDC. They protect against some of the larger particles in wildfire smoke, but not from smaller particles in smoke that can damage the lungs. In addition, one-strap paper dust masks and surgical masks, worn alone, are not recommended for wildfire smoke protection.
It is recommended that people who have to be outdoors in wildfire affected areas wear fit-tested, NIOSH-approved N95 or P100 respirators, and the CDC notes that properly fitted N95 respirators can "provide protection from wildfire smoke and from COVID-19 for the individuals wearing them." To help prevent the spread of COVID-19 to others, N95 masks without valves are recommended. If an N95 mask with a valve is your only option for wildfire smoke protection, consider covering the valve with tape or wearing a surgical mask over the N95 when around others, as recommended by John Balms, M.D. at UCSF. KN95 respirators can also provide protection from particles in wildfire smoke (see our Top Pick among KN95 masks, which was tested by the CDC).
Join today to unlock all member benefits including full access to all CL Answers and over 1,400 reviews.
Join NowAlready a member? Sign In Here.
Join now at www.consumerlab.com/join/




Submit your comment
This feature is restricted to active members.
Join now to add comments and get all member benefits, including over 1,400 reviews.
Join NowAlready a member? Sign in here.