Quick Summary
-
Does melatonin work?
Melatonin supplements can help you fall asleep sooner, although not necessarily for longer, when taken before bedtime (30 to 60 minutes before for regular pills; 20 minutes before for fast-dissolve pills, chewables, and liquids and chewables). Studies suggest it may help with sleep issues during and after menopause, in children with autism spectrum disorder, and in people with Parkinson's disease. Melatonin may also reduce migraine and primary stabbing headache, alleviate symptoms of stomach ulcer, gastroesophageal reflux disease (GERD), and functional dyspepsia (stomach pain not caused by an ulcer), and reduce anxiety associated with medical procedures (see What It Does). -
How much melatonin to take:
Melatonin is a hormone; use it only as needed, not every night. Try the lowest dose that will work for you, starting with about 1 mg or less. If that doesn't work, try 3 mg. Some products contain greater amounts, such as 5 or 10 mg, which may be more than you need and can leave you groggy and have other negative effects. Timed release products may help you not just fall asleep but also stay asleep, but they won't help you stay asleep as well as a prescription sleep medication.
While nuts, including pistachios, almonds, cashews, Brazil nuts, chestnuts and peanuts, contain melatonin, the amount is much lower than doses shown to be effective.
Taking small to moderate doses of melatonin from supplements does not appear to reduce the body's own production of melatonin, although other factors (such as taking high-dose vitamin D) may decrease your body's natural levels of melatonin (see ConsumerTips™: What to Consider When Using). -
What did CL's tests of melatonin supplements show?
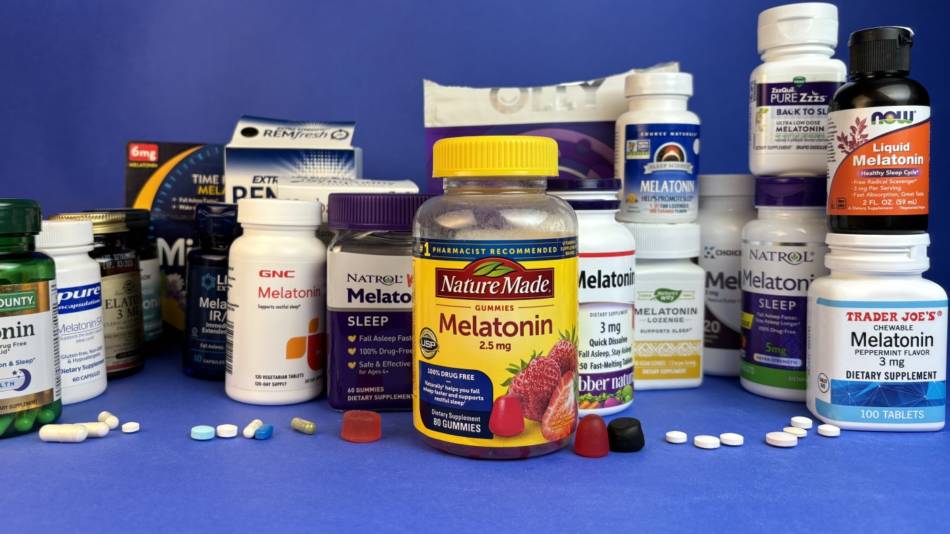
In laboratory testing, all the melatonin supplements were found to contain their listed amounts of melatonin within a reasonable margin. This was better than what ConsumerLab found in 2020, when one product contained nearly twice its listed amount of melatonin; and it is better than other researchers have found when sampling the market (see Quality Concerns).Our cost comparisons show you could spend as little as 1 cent to over 60 cents per milligram of melatonin (see What CL Found and How Products Were Evaluated).
-
Best melatonin supplement?
Among 20 CL Approved products, CL selected Top Picks for low, moderate, high, very high dose and time release melatonin, as well as a product for children and one for pets. These products represent superior quality and value. -
Melatonin safety and side effects:
Melatonin supplements, taken in doses up to 3 mg per day, short-term, appear to be generally safe for adults. Drowsiness may occur, often for about six hours after taking melatonin (although it may last longer if controlled-release, higher dose products are used). Impaired mental alertness and balance, headache, dizziness, and nausea may also occur. Higher doses of melatonin may affect blood pressure, aggressiveness, blood clotting, seizure activity, and, at very high doses, ovulation, depression, and schizophrenia. Rarely, heart palpitations or premature ventricular contractions (PVCs) have been reported. Melatonin can interact with certain foods and increase the effectiveness of certain medications (such as sedative or sleep medication) or decrease the effectiveness of others (such as blood pressure medications). Certain drugs (and even caffeine) may increase the amount of melatonin you absorb from supplements. Long-term use is associated with an increased risk of bone fracture and slower healing after a fracture occurs. It is best to use melatonin "as needed" rather than on a regular basis (see Concerns and Cautions).