Our Members Asked:
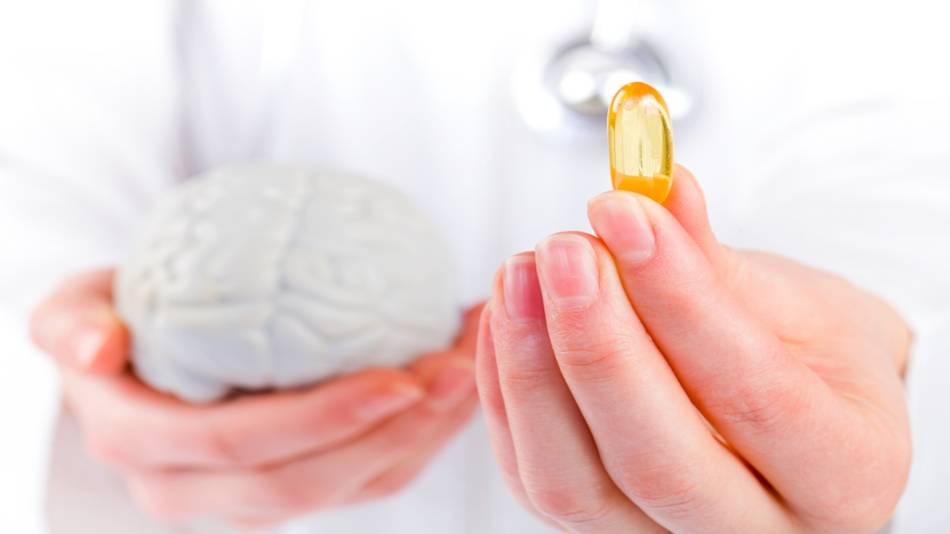
Do any supplements, foods or lifestyle modifications help with brain function, like memory and cognition?
Answer:
There is preliminary evidence that certain supplements modestly improve various aspects of memory or cognition. These benefits include boosting memory in people who do not have memory problems as well as improving memory or cognition in people with age-related cognitive decline, Alzheimer’s disease, and other forms of dementia. At the same time, several supplements have not been shown to help with memory or cognition.
In addition, certain foods, diets, and lifestyle changes have been associated with improvements in cognition or a decreased risk of dementia.
Sign in as a member to find out if any of the following supplements help with brain function: Acetyl-L-carnitine, apoaequorin (the main ingredient in Prevagen), ashwagandha, bacopa, beta-alanine, choline, cocoa flavanols, coenzyme Q10, coffee or coffee extracts, cranberry, curcumin (from turmeric), fish oil, ginger, Ginkgo biloba, grape seed extract, green tea, huperzine A, inositol-stabilized arginine silicate, iron, ketones, L-arginine, lion's mane, lithium (low dose), lutein and zeaxanthin, magnesium, magnolia bark extract, medium chain triglycerides (MTC), melatonin, multivitamins, nicotinamide riboside, phosphatidylserine, plasmalogen, PQQ (pyrroloquinoline quinone), prebiotics (such as Sunfiber), probiotics, soy isoflavone genistein, spermidine, sulforaphane, vinpocetine, and vitamins B-12, D, and E.
Also find out which foods (such as eggs), diets (such as the Mediterranean and MIND diets) or lifestyle modifications may be beneficial, and learn about ingredients promoted for memory and cognition that are not permitted to be sold as supplements.
Join today to unlock all member benefits including full access to all CL Answers and over 1,400 reviews.
Join NowAlready a member? Sign In Here.
Join now at www.consumerlab.com/join/

.jpg?size=thumbnail)









Submit your comment
This feature is restricted to active members.
Join now to add comments and get all member benefits, including over 1,400 reviews.
Join NowAlready a member? Sign in here.