Our Members Asked:
How much calcium do you need each day, what forms are best, and how much is too much?

Answer:
It is important to get an adequate amount of calcium, as it is essential to maintaining your bones and plays critical roles in nerve transmission, muscle contraction, and your cardiovascular system. Calcium is best obtained naturally from foods, but supplementing with calcium can help when intake is otherwise not sufficient. Be aware that getting too much calcium from supplements is associated with certain risks.
How much calcium do you need?
For women over age 50 and men over age 70, the recommended daily intake of calcium is 1,200 mg from food and supplements combined — although it's best to get most of this from foods. For women under 50 and men under 70, it's 1,000 mg daily. Children ages 9 to 18 have the largest daily requirement: 1,300 mg, while younger children need less. The Daily Value for calcium (which is used in product labeling) is 1,300 mg and was developed to address the group with the greatest requirement for calcium — adolescents and teenagers.
If you can get most of your calcium from food, then it's best to limit your intake of calcium supplements to just the amount you need to meet the recommended intake. To get an idea of how much calcium is in common foods, see How much calcium do you already get from food? section of the Calcium Supplements Review.
Experts believe that one can't absorb more than about 500 mg of calcium at time, so foods or supplements with higher doses may provide too much calcium. For instance, if you drink a cup (8 fl oz) or more of milk that is fortified with calcium at a time, this milk may provide you with too much calcium. On the other hand, a cup of lactose-free milk that is not "calcium fortified," will naturally provide about 30% of the Daily Value for calcium (390 mg based on the new DV), which is not too much.
Similarly, if you decide to take a calcium supplement, it is generally felt that calcium supplementation should not exceed 500 mg per dose and no more than 900 mg per day. Extended-release calcium supplements might help increase the amount absorbed from higher doses, but 600 mg per dose may still be more than you need.
If you have a cup of milk along with calcium-containing foods or supplements, you may be getting more calcium than you can absorb at one time.
There is a myth that calcium intake needs to be increased when taking a protein supplement. There is no evidence that healthy adults need to increase calcium intake when taking protein supplements, as explained in the Concerns and Cautions section of our Protein Supplements Review.
What's the best source of calcium?
Calcium from foods
In general, it's preferable to get most of your calcium from foods that contain it naturally, rather than from supplements or calcium-fortified drinks and foods like orange juice, certain lactose-free milks, and nearly all plant-based milks (such as soy and almond milks) — which are like taking a supplement with food. A common form of calcium added to these beverages, as well as to gummy and liquid supplements, is calcium phosphate or tricalcium phosphate. Calcium from all sources counts toward the Tolerable Upper Intake Level (UL) — above which the risk of adverse effects increase — but it is rare to exceed this limit from natural foods alone. The UL is 2,000 to 2,500 mg for adults, 3,000 mg for adolescents and teenagers, 2,500 mg for children over age 1, and 1,000 to 1,500 mg for infants.
Dairy:
Dairy foods serve as the primary food source of calcium for many people. A cup of milk or yogurt provides 300 to 400 mg of calcium — about one-third of the daily requirement. It can be a challenge to get sufficient calcium from your diet if you cannot eat dairy foods, since they are typically the major source of calcium. However, other foods, including plants and meats, can provide significant amounts of calcium — although one must be aware that calcium is not well absorbed from certain plant-based foods.
Plant-based foods:
Many plant-based foods are rich in calcium, but calcium bioavailability from these foods can be reduced by their contents of oxalate and phytate, which inhibit calcium absorption. For example, calcium bioavailability is low from spinach, which is high in oxalates: you only absorb about 6 mg of the 115 mg of calcium per ½ cup serving.
In contrast, calcium absorption is high from low-oxalate vegetables such as kale, broccoli, and bok choy — these provide about 25 to 40 mg per ½ cup serving. An exception is soybeans, which are rich in calcium but, despite also being high in oxalate and phytate, have relatively high calcium bioavailability (Weaver, Am J Clin Nutr 1999). A ½ cup of cooked soybeans provides about 125 mg of calcium. Tofu (which is made from soybeans) provides 160 mg of calcium per ¼ firm block — although much of this is from calcium which has been added as a setting agent. Beans, which are rich in calcium but also in phytate, have substantially lower calcium bioavailability; among beans, white beans are highest in calcium — you'll get about 25 mg per ½ cup serving.
Nuts and seeds are also rich in calcium. For example, you can get about 80 mg of calcium from a 28-gram serving of almonds or just a tablespoon (9 grams) of sesame seeds.
Although soybeans and almonds are rich in calcium, be aware that most of the calcium in soy and almond milk products is added, which is why the amounts can be comparable to that in milk. (See how much added calcium is in plant-based milks in the What CL Found section of our Plant-Based Milks Review.) Added calcium in fortified foods and drinks count as supplemental calcium — see below about limiting the amount of calcium you get from supplements.
Meats:
Meat and poultry also provide calcium — about 120 mg per 100 gram serving. Fish meat contains less calcium, but, because they include small bones, sardines are very rich in calcium (600 mg per serving) as is canned salmon, which includes softened bones (200 mg per serving) (USDA National Nutrient Database).
Water:
Water contains some calcium, although the amount is generally small. Tap water contains only about 12 mg of calcium per 8-fl. oz glass, so that 6 glasses provides only about 7% of the adult daily requirement for calcium. Bottled mineral water can contribute more (e.g., about 49 mg per glass), while spring water contributes less (5 mg per glass) and purified water contributes only negligible amounts (Moor, HSS J 2006). Keep in mind that reverse osmosis filtering removes nearly all calcium from water (Kamalapriya, Cureus 2023) and even water filter pitchers may remove calcium from water, particularly those designed to remove nearly all total dissolved solids (TDS) (see the What CL Found section in our Water Filter Pitchers Review).
Calcium from supplements
Calcium supplements, if chosen and used properly, can help fulfill the daily requirement for calcium. However, before you turn to supplements, try to get as much calcium from your foods, because calcium's greatest benefits occur when it's consumed from natural sources.
Similarly, potential risks of calcium supplementation are minimized when taking lower daily amounts. If you are considering taking a calcium supplement, be sure to calculate how much calcium you are already getting from food, and from other sources, such as over-the-counter antacids, and then only supplement with the amount you need to meet the recommended daily intake.
As noted above, it is best to limit a single dose to 500 mg of calcium. Be aware that some supplements, like Viactiv, provide more than that per serving. Also, be sure you are getting adequate vitamin D, as this increases the absorption and proper utilization of calcium. Taking a calcium supplement containing 400 to 800 IU of vitamin D, for example, may help and is quite safe. See CL's Top Picks for calcium supplements, including those with vitamin D.
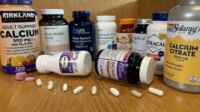
Forms of calcium in supplements:
Calcium carbonate is the most common form used in supplements. Other forms such as calcium citrate may be better absorbed, but the amount of calcium in this form, as well as other forms such as calcium lactate and calcium gluconate, is small compared to calcium carbonate, meaning more pills or larger pills need to be taken. Also, these forms tend to cost more, although it is less important to take them with food (calcium carbonate should be taken with food as this stimulates the production of acid needed to make the calcium in this form more absorbable).
Calcium hydroxyapatite is a form of calcium derived from cow bone and typically includes an array of other minerals as well as bone proteins. However, it is not necessarily a safer form of calcium, as explained in the Calcium Supplements Review.
Calcium is sometimes sold as part of a "food-based" or "plant-based" formula, such as AlgaeCal (Basic). AlgaeCal contains calcium, magnesium and trace minerals derived from algae with added vitamin D. AlgaeCal Plus also includes added vitamins C and K, boron, and additional magnesium. Testing by ConsumerLab.com in 2011 found AlgaeCal Plus to contain a higher amount of lead (a toxic heavy metal) (5.2 mcg per daily serving of 4 capsules) than many other calcium-containing supplements. Testing in 2017 found less lead, although still higher than acceptable to CL, but also less magnesium than listed on the label.
Studies sponsored by the makers of AlgaeCal found that it increased bone mineral density in healthy men and women, although there were weaknesses to the study design. There do not appear to be any clinical studies comparing the effects of AlgaeCal to other forms of calcium, such as calcium carbonate or calcium citrate nor to other calcium + vitamin D supplements.
For more about getting the right amount of calcium, sources and different forms, and our tests of popular products, see the Calcium Supplements Review.
Keep in mind that not all supplements that contain calcium are intended to boost calcium levels. Calcium-d-glucarate is a form of glucaric acid (a naturally occurring substance found in certain fruits and vegetables). It is this glucaric acid portion of the compound (and not the calcium portion - which is only 12% the compound's weight) that appears to be responsible for its activity, as it can inhibit the enzyme beta-glucuronidase and, thereby, increase glucuronidation and excretion of potentially toxic compounds. Although it has been promoted for "detoxifying" effects, as well as for lowering estrogen levels and preventing cancer growth, these applications are, for the most part, suggested only by laboratory and animal studies, not clinical studies in people.
Fruits and vegetables such as oranges, broccoli, cabbage and potatoes contain small amounts of glucaric acid - between 1 mg and 4.5 mg per 100 g serving (a little less than one cup) (Dwivedi, Biochem Med and Metabol Biol 1990). These are relatively small amounts compared to what has been used experimentally. A diet rich in these foods was not found to decrease beta-glucuronidase activity in people (Maruti, Cancer Epidemiol Biomarkers Prev 2008).
Is too much calcium harmful?
Although maintaining adequate calcium intake is important for bone and cardiovascular health, getting too much calcium — particularly from supplements — can be harmful. In general, getting more than 1,000 mg of calcium per day from sources other than food has been linked with certain health risks.
One study determined that the risk of heart attack with calcium supplementation tends to be greater in those already getting more than 805 mg of calcium from their diet (excluding supplements). Getting too much calcium from supplements can also increase the risk of arterial calcifications.
Use of calcium supplements may increase the risk of dementia in elderly women who have evidence of cerebrovascular disease or who have a history of stroke.
There is mixed evidence as to whether calcium from supplements increases the risk of age-related macular degeneration (AMD). One study found that regularly consuming too much calcium from supplements or antacids was associated with a higher risk of developing AMD. In contrast, another study did not find a higher risk of AMD with supplements. In fact, it found that women with high intake of calcium from supplements had a lower risk of a particular form of AMD (neovascular or "wet" AMD) than those who did not supplement with calcium. Calcium from foods does not appear to have a negative effect on AMD and may, to some extent, reduce the risk of AMD. For details, see the What It Does section of the Calcium Supplements Review. For supplements that can help with AMD, see the Vision Supplements Review.
While not conclusive, some observational studies have found an association between high total calcium intakes (>1,500 mg per day) and an increased prostate cancer risk. Since most men over the age of 50 can probably get all the calcium they need from foods, calcium supplement intake should be limited. For information about products for an enlarged prostate, see Prostate Supplements Review.
Too much calcium also increases the risk of kidney stones, and 5% to 8% of men and women have idiopathic calciuria (too much calcium in the urine for unknown reasons), which is a risk factor for kidney stones. Even 600 mg of calcium may be too much for such people, despite a diet somewhat low in calcium.
Can other supplements or OTC medicines contribute to calcium intake?
Many over-the-counter antacids contain calcium carbonate, which can contribute to your daily calcium intake. For instance, it can be easy to exceed the recommended daily intake for calcium if you take several tablets of Tums per day. For this reason, it's important to consider how many tablets you are taking and what strength they are (i.e. regular, extra strength, "ultra," etc.).
Multivitamins may also provide calcium, though the amount is typically less than 20% of the 1,000 to 1,200 mg adult daily requirement, so there is little safety concern with this amount of calcium from a supplement if you're not getting quite enough from your diet. However, if you're sure that you get sufficient calcium from your diet and want to avoid getting more from a multivitamin, there are multivitamins that contain only tiny amounts (under 20 mg) of calcium — usually as incidental part of another ingredient in the supplement. You can easily find products like this by comparing the amounts of calcium listed in the "Minerals" comparison table of the Multivitamin/Multimineral Supplements Review.
Can calcium interact with other supplements or medications?
Calcium and magnesium can compete with each other for absorption. Consequently, it's best to take them at separate times, especially if you need to take large amounts (250 mg or more) of either of these. For more details, see the What to Consider When Using section of the Calcium Supplements Review, which includes our Top Picks among calcium supplements.
For the same reason, it's also best to take other minerals, such as iron and zinc, at a different time of day than calcium. Taking calcium can inhibit iron absorption by as much as 62%, although this depends on the dose of calcium. This interaction is of greatest concern for younger women, as they are the most likely to suffer iron deficiency. For more details about this interaction and how to avoid or minimize it, and about other minerals and foods that can inhibit iron absorption, see the What to avoid when taking section of the Iron Supplements Review.
It is best to avoid taking calcium citrate along with medications that contain aluminum (such as aluminum hydroxide in the antacid Maalox), as citrate can increase aluminum absorption. If you need supplemental calcium and an antacid, consider taking Tums, which contains calcium carbonate rather than aluminum hydroxide. Keep in mind that calcium citrate can also increase absorption of aluminum from foods. Although this is unlikely to be a concern in individuals with normal kidney function, this might be a concern for people with kidney disease. See the Concerns and Cautions section of the Calcium Review for more details.
Calcium can also interfere with the absorption of certain medications, including antibiotics in the fluoroquinolone and tetracycline families, levothyroxine (Synthroid), and bisphosphonate medications such as alendronate (Fosamax). Taking calcium supplements along with thiazide diuretic drugs such as hydrochlorothiazide (Esidrix, Ezide, Microzide) can increase the risk of hypercalcemia. See the Concerns and Cautions section of the Calcium Review for more about these interactions, including how to separate doses to avoid interactions.
For more information about calcium see our Calcium Supplements Review, which includes our tests and reviews of popular calcium supplements and our Top Picks among them.
Join today to unlock all member benefits including full access to all CL Answers and over 1,400 product reviews.
Join NowAlready a member? Sign In Here.
Join now at www.consumerlab.com/join/