Answer:
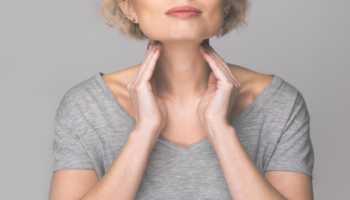
The thyroid, a small gland located at the front of your neck, produces hormones that help control breathing, heart rate, digestion, and body temperature. When thyroid activity is low, a condition called hypothyroidism develops. Hypothyroidism can result from an autoimmune condition known as Hashimoto's disease, a disease in which the immune system attacks the thyroid gland and prevents it from making enough hormones. On the other hand, thyroid activity can be high — a condition known as hyperthyroidism. Hyperthyroidism can result from an autoimmune condition known as Grave's disease, a condition marked by overproduction of thyroid hormones.
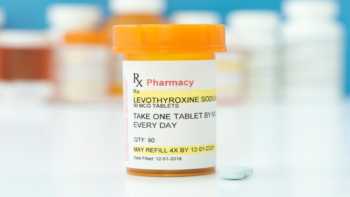
In most cases, these thyroid conditions are treated with medications such as thyroid hormone replacement (e.g., levothyroxine) for hypothyroidism and antithyroid drugs (e.g., methimazole or propylthiouracil) or surgery for hyperthyroidism. However, since some evidence shows that certain dietary supplement ingredients may also help with thyroid conditions, supplement manufacturers have marketed products designed for "thyroid health."
Ingredients in "thyroid" supplements include iodine (sometimes incorrectly marketed as "nascent iodine"), selenium, zinc, acetyl-l-carnitine, ashwagandha, guggul, and black seed. While some of these supplement ingredients may be beneficial in certain people, in many cases, these supplements are not needed, and they may do more harm than good. Furthermore, some supplements marketed for "thyroid support" contained actual thyroid hormones, which can pose a risk if the hormone amounts are less or more than needed.
Sign in for more details about the potential benefits and possible safety concerns of ingredients and supplements for thyroid health (such as Thyroid Care Plus from Terry Naturally) and desiccated thyroid extracts (such as Armour Thyroid and NP Thyroid), as well as information about ingredients such as alpha-lipoic acid, soy, resveratrol, quercetin, calcium, vitamin D, iron, and magnesium hydroxide, which may impair thyroid function or interact with prescription medication used to treat thyroid conditions, and whether eating cruciferous vegetables can impair thyroid function. Also learn about situations in which thyroid medication appears to be overprescribed.
Join today to unlock all member benefits including full access to all CL Answers and over 1,400 product reviews.
Join NowAlready a member? Sign In Here.
Join now at www.consumerlab.com/join/