Quick Summary
-
Health benefits of calcium:
It is important that you get an adequate amount of calcium, as it is essential to maintaining your bones and plays critical roles in nerve transmission, muscle contraction, and your cardiovascular system. In fact, getting sufficient calcium each day (1,000 to 1,200 mg for adults) from your diet (i.e., not all from supplements) may decrease your risk of dying from cardiovascular disease. For details, see What It Does. -
Good sources of calcium:
You may already get enough calcium in your diet from dairy, beans, green-leafy vegetables, and other foods. With the exception of girls ages 9 to 18, most individuals take in enough calcium from what they eat. For the recommended intakes of calcium and to learn how much you may already get from food, see What to Consider When Using. -
Safety and side effects of calcium supplements:
If you're not getting enough calcium from your diet, supplements can help. Calcium supplements have shown some modest benefits for postmenopausal women, particularly those on hormonal therapy after hysterectomy (see What It Does). But be careful! Getting too much calcium from supplements (generally over 1,000 mg per day-or if taken when you already get at least 805 mg of calcium from your diet) may increase the risk of heart attack and stroke. There is mixed evidence as to whether calcium intake affects prostate cancer risk. Calcium supplements also increase the risk of kidney stones in postmenopausal women. See Concerns and Cautions for more information. -
What's the best form of calcium?
Calcium carbonate is the most common form of calcium in supplements, but other forms, such as calcium citrate, may be better absorbed if you have low levels of acid in your stomach. A slight downside to these other forms is that they require larger pills (or more pills) to get the same amount of calcium compared to calcium carbonate. Other forms include calcium malate, triphosphate, and hydroxyapatite (derived from cow bone), as well as "plant-based" calcium such as Aquamin and AlgaeCal (derived from algae). For more about the pros and cons of each form, see What to Consider When Using. -
How much calcium to take?
Since you can't absorb more than about 500 mg of calcium at a time, consider limiting intake from supplements to 500 mg or less at a time and, certainly, no more than 1,000 mg total per day. Also, be sure you are getting enough vitamin D, as it is necessary for your body to absorb and utilize calcium from both foods and supplements and may reduce some of the risks associated with calcium supplements. Vitamin D is in many of the supplements tested in this Review. For extensive information about vitamin D, see the Vitamin D Supplements Review. Which calcium supplement is best?
Not all supplements are properly made and live up to their ingredient claims. In fact, one combination product failed our tests because it provided only 81% of a promised key ingredient (see What CL Found and How Products Were Evaluated). ConsumerLab selected several Top Picks among calcium-containing supplements that were Approved in testing— some of which provide a good dose of calcium for just pennies a day. Use our Results table to narrow in on an Approved product that provides the right amount of calcium and other ingredients (e.g., magnesium, vitamin D, vitamin K, and/or boron) to meet your needs.
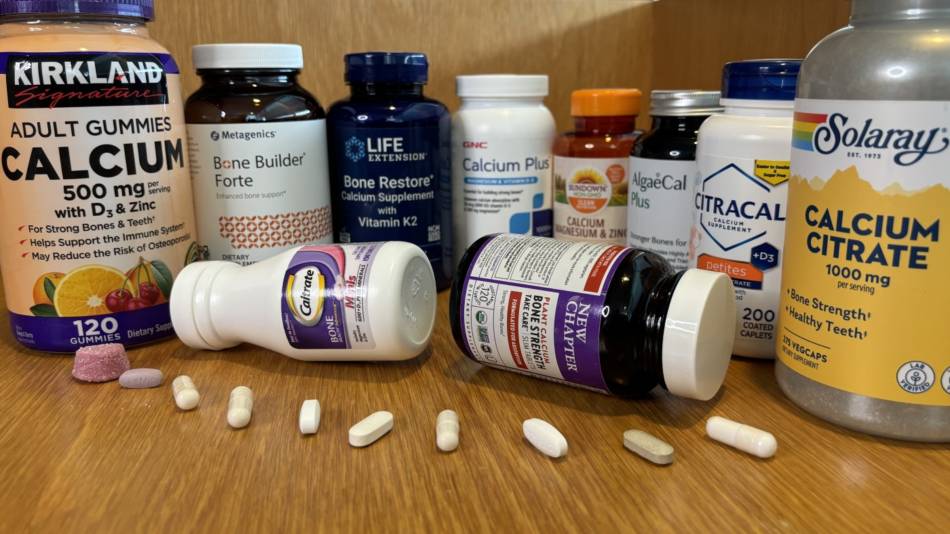
Brands tested in this Review are AlgaeCal, Bayer Citracal, Caltrate, GNC, Kirkland, Life Extension, Metagenics, New Chapter, NuBest, Solaray, Sundown, and USANA. Other products discussed include Jarrow BoneUp, Swanson Calcium Aspartate, EZorb Calcium, Webber Naturals Calcium Citrate Vitamin D3, and Country Life Magnesium Complex.)-
When and how to take calcium?
If your calcium supplement includes vitamin D and/or vitamin K, take it with the meal that contains the most fats and oils, as this may increase absorption of those vitamins. Otherwise, you can take calcium with any meal, but it may be best not to take it at the same time as other mineral supplements, as they may compete for absorption. If you are taking calcium citrate, you may be able to take it with or without food. Follow the directions on the supplement label (see How to Take).